The Stages of Change - GF Edition

This is a companion article to “Gluten-Free Success.” I started out writing Gluten-Free Success, but a quote from Vishwas Chavan sent me down a rabbit hole. That trip resulted in this article. Thanks for riding along.
Al Klapperich
BRAIN: "What's that noise? Why are those bushes rustling? Is it a wild animal getting ready to attack us? DANGER!"
When confronted with change, our brain can't predict the outcome, so it triggers the"flight or fight" response. Faced with uncertainty, we find ourselves distracted, anxious, and fearful. This heightened state decreases decision-making abilities, reduces memory, and elevates anger; not always conducive for clear, thoughtful consideration. The human brain is an astounding organ. Not only does it need to maintain order, but it also manages adaptation. We may not notice it, but our brains are continually changing in response to our ever-changing environment; the scientific name for this process is neuroplasticity. This adaptability enables our species to thrive and survive all kinds of adversities. The trick is to use our innate adaptability to our advantage. However, this metamorphosis requires a lot of effort. When transitioning into the gluten-free lifestyle, there are a lot of changes, unknowns, and unpredictable outcomes. Yes, our brains are going to freak-out. We are replacing old comfortable habits and behaviors with new, unfamiliar ones. Those old behaviors have become almost automatic; requiring little to no thinking. We have had a lifetime to build those neural pathways in our brains.
Neural pathwhats? The pathways along which information travels through the nerve cells of the brain. When we say or do things repeatedly, that information in our brain travels the same path. Think about a hiking trail in the woods - as the path receives more traffic, it becomes better defined, well worn and effort-less to travel - the same thing happens in our brains. When we start our gluten-free lives, we are blazing new pathways. This requires us to be conscious, and purposeful in our efforts.
Over the years, scientists and mental health care professionals have developed many thoughts and theories about the brain, the process of change, and human behavior. Of the many behavioral change models that exist, the most prevalent are Learning Theories, Social Cognitive Theory, Theories of Reasoned Action and Planned Behaviour, Transtheoretical Model of Behavior Change, The Health Action Process Approach and the BJ Fogg Model of Behavior Change. Each model has its own set of strengths and weaknesses. That's not something we'll be discussing here. We will be exploring the Transtheoretical Model of Behavior Change (TTM) - also known as The Stages of Change. I chose this method because it made sense to me, it seemed logical and fit my personality and way of thinking. Will it be a fit for you? I don't know the answer, but keep reading you might be surprised.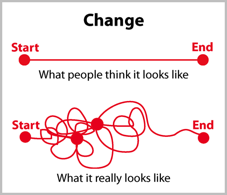
- The Stages of Change - when change occurs.
- Pre-Contemplation: No action for six months.
- Contemplation: Intention to act within six months.
- Preparation: Intention to act within 30 days
- Action: Experiencing change for less than six months.
- Maintenance: Experiencing change for more than six months.
- Decisional Balance (Pros & Cons) - why we change.
- Weigh the Pros (advantages) and Cons (disadvantages) of changing.
- Pros and Cons are independent of one another. Can be high in one - low in another. High in both, or low in both.
- Pre-Contemplation stage - the Cons of changing out-weigh the Pros
- From Pre-Contemplation to Contemplation - the Pros consistently increase
- From Contemplation to Action - the Cons consistently decrease
- Pros begin to outweigh the Cons before we take action.
- The key: double-up the focus on increasing the Pros of changing.
- Self-efficacy (Confidence & Temptation) - confidence to execute change.
- Confidence is low and tends to grow as we progress through the stages. Inversely, temptation lessens.
- We see the biggest jump in confidence in the Action and Maintenance stages
- Confidence and Temptation tend to be balanced during the Action stage.
- The Processes of Change - how change occurs.
- Describes the basic pattern of activity we experience as we process change.
Pre-contemplation
In this stage we do not know we have to change, or we do know, but simply do not want to. When it comes to the effects of gluten, there's a wide spectrum. [This stage casts a wide net over the gluten-free community.] In most cases, people with gluten-related disorders have experienced some ill-health - be it long-term or short-term. We know something is wrong, but haven't been diagnosed or have been misdiagnosed. Maybe we think our state of being is perfectly normal because we've always been that way - our entire family is that way. If we have silent celiac disease [have no symptoms], a diagnosis will catch us completely by surprise. We may have a diagnosed family member urging us to get tested, but we brush them off like a pesky mosquito. In this stage, we don't want to hear that gluten could be a problem for us.
"Give up my bread/pizza/beer? No way, I'd die without it." "Just because you have problems with gluten, doesn't mean that I do." "Bah, my sensitive stomach has nothing to do with gluten." If that sounds like denial, yes, it probably is.
To move past this stage, we must somehow become aware that a problem exists and accept that we must address it. We may come to this realization on our own after we've been given testing results from our healthcare professional, or we finally listen to our family and friends. The mere fact that we are "thinking about it" is forward progress!
Contemplation
This stage finds us realizing the value in making the change; the mental gears have been turning, and we are getting ready. We have thoughts of "Yeah, I get that gluten-free is important" but the key is to personalize them by thinking "I need to be gluten-free." Here we start to acknowledge the problem and take ownership. Our minds are now open to new ideas and information. We may begin asking questions of friends and family who have already gone gluten-free. The trick is discovering the trigger - the event, the person, the emotion, the reason we flip the switch. We begin to explore the possibilities about what we need to do and if it will be worth the effort. These thoughts can be fleeting or last a lifetime. The bottleneck in contemplation is getting stuck in a loop of weighing the benefits against the costs of making the change. We never feel ready to commit. Deep down we know change is needed, but we can't make it happen. To help organize and visualize our thoughts, sit down with a pencil and paper - list all the pros on one side and the cons on the other. When we encounter obstacles, identify ways to overcome them.
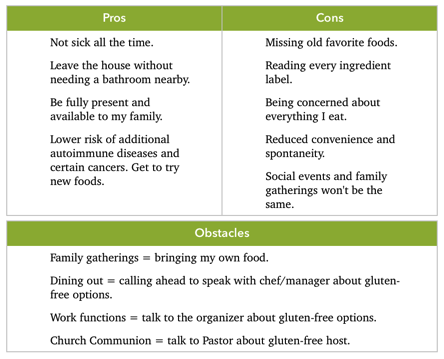
With everything that's going on, our emotions may inspire us to act immediately. Sometimes this causes us to jump right into the Action stage - bypassing one of the most important stages - Preparation. Action without perparation can lead to disaster.
Preparation
We've made the decision to change, now we must figure out how to do it.
SELF: "What do I need to do to prepare myself to make this transformation happen?"
Any successful outcome begins with forethought and planning. We are creating a plan of action; a road-map if you will. Put it in writing, draw pictures with circles and arrows, create a wall-sized vision board, save the plan as your device's wallpaper or desktop picture as a constant reminder - do whatever generates the greatest impact. Begin gathering the tools and resources to help us navigate our gluten-free journey. One of the most effective resources is a local support group; seek out your nearest group - inquire about their meetings (when, where, how often, etc.) - better yet, join and attend a meeting. Start building a library of trusted books and websites. This stage is about building our knowledge and confidence, preparing us for gluten-free success. Think about all the possible ways we cross paths with gluten. Cupboards, pantries, refrigerators, freezers, silverware drawers, cutting boards, toasters, kitchen utensils, counters, medication, hair and personal care products, family gatherings, parties, social functions, restaurants, medical and dental procedures - the list is staggering. All of these things and more need our attention. It's better to have a plan of action so we can be PROactive instead of REactive. Some of our very first actions begin appearing. The key to mastering this stage is a commitment to all the effort, planning, and researching. We must be ready to go all-in. Being "sort of " gluten-free is like being "a little"pregnant.
Action
It's game day! We move from thinking and planning to doing. We've done the risk/benefit analysis and committed to making the leap - we've made a plan, and now it's time to act! It's here where real change starts happening.
We go on a gluten-round up at home - seeking out and removing all sources of gluten. If we can't do a 100% GF house, we gather and store all the gluten in designated areas. Empty and clean out every cabinet and drawer [see all the crumbs in the silverware drawer? YIKES!] Clean the fridge and stove, get a new toaster, cutting boards, and colanders. Join and actively participate in the local support group [if you haven't done so already]; we truly need that face-to-face support. Read the mountain of gluten-free books sitting on the coffee table. By following our initial action plan, we'll be making significant modifications to our routines, environments, our relationships, and of course ourselves. That's the whole idea, right?
As expected, this stage will require every ounce of commitment we can muster. We may find ourselves being pushed and pulled to the very limits. Sadly, some of this stress may come from those closest to us. We need to hold fast to the course we've plotted out; for our own health and wellbeing. If we find ourselves drifting or blown off-course refer back to the plan of action we created. Keep finding acceptable alternatives and focusing on our "cans" instead of "can not's" It's necessary to acknowledge and celebrate the progress and victories along the way - no matter how seemingly insignificant we think they are. Anything that moves us forward toward our goal is a success! We also need to recognize the failures, not to chastise ourselves, but to learn from them. If we know why something happened, we can prevent it from happening in the future.
Maintenance
The maintenance stage is about sustaining the momentum we started in the beginning. At first glance, we think the hardest part of the change process is the initial startup. True it's tough, but maintaining the change long-term is the most challenging part of the process; it's also the most important. At this point, our new lifestyle is on its way to being established, things are starting to become routine. Confidence is increasing. Certain memories of our past lives are starting to fade. Complacency is our enemy because of the possibility of slipping into our old lifestyle may be lurking in the background. Dramatic life events such as a job change, breakdown of a relationship, a death make us vulnerable. These events can beckon us back into our old habits. While our original plan serves us well, we keep optimizing it to address past mistakes and handle any situations we didn't expect at the start. View these challenges as an opportunity to advance your skills, knowledge, and confidence. This continued growth pushes us ever closer to the next stage. Perhaps more work on label reading is needed because small amounts of gluten are slipping below our radar despite our diligence. We didn't think about our church's communion hosts containing gluten. Our high school class reunion is coming up, maybe we could volunteer to be on the planning committee to have a voice in food options.
Pro tip: Get involved in planning activities. This gives us an opportunity educate and make positive changes from the "inside."
Because of our new gluten-free lifestyle, our bodies are adjusting, adapting, and healing - mentally and physically. After gluten reactions subside, we may discover other problematic foods. Of course, this will require additional tweaks to our plan. The diets to obtain optimal health are as unique as our fingerprints. It can take some time resolve additional food sensitivities. As we settle into maintaining our new life, we may struggle with keeping the fire lit; we run the risk of losing the intensity. If we haven't participated in a local support group already, make it a priority. Surrounding ourselves with like-minded individuals can help keep us motivated. Fellow members walk our walk, talk our talk, share the same struggles and joys.
Termination/Adoption
We started out telling ourselves "I can't", then "I might", followed by "I will", "I am", "I am still", and now finally "I have". It's been a long road on our way to change. After spending at least two years in the Maintenance stage, we find ourselves sliding into the Termination/Adoption stage. At this point, we don't have to think so hard about what to do; we know what to do. Our daily activities come to us naturally; they become second nature, almost as automatic as breathing. We have confidence in our knowledge and abilities. Sure, we may miss certain aspects of our former life, but the desire to return to that unhealthy and sickly life has dissipated. Our transformation from gluten-full to gluten-free has come to fruition. Our new life has become our "new normal." We started out as a caterpillar and came out the other side as a butterfly. Well done. A proud moment for sure. This does not mean we stop our personal evolution process! No, we keep moving forward. We look for new and more adventurous goals. Now is the time to dream and plan for things we never thought possible in our former life. Perhaps we have a strong desire to share what we've learned to help others. Starting your own support group or volunteering at your current group is an excellent choice. Maybe we participate more in online discussion boards or Facebook groups. Possibly start our own blog or website. There are many ways to boost our gluten-free advocacy to the next level. Maybe your new goals have nothing to do with gluten. Perhaps you want to train for that 5K, 10K, or Half Marathon you've always wanted to do? What about music or voice lessons? Now would be a great time to start that writing project. The possibilities are only limited by your imagination. Prochaska estimates only about 15 to 20 percent of the people make it to this stage. If you find yourself falling back into previous stages, don't panic. Be gentle with yourself. Figure what stage you're in - go back to your game plan, see if it needs a bit of tweaking and renew your commitment to moving forward. Ask for help. Never give up.
Relapse/Lapse
Not an official stage of Prochaska and Di Clemente's model but some valuable insights can be learned here. Note: Repeated gluten exposure is a serious health risk for those with a gluten-related disorder. There is an important difference between relapse and lapse (also known as a slip). A lapse or slip is a rare, quick and temporary return to the behavior/lifestyle we've been trying to leave behind.
Example: while attending a birthday party, we have a piece of gluten birthday cake.
A relapse is a complete and total return.
Example: we tell ourselves the gluten-free lifestyle is too hard and go back to eating gluten.
Gluten is so pervasive in our society, no matter how hard we try, we will likely be faced with a gluten exposure at some point. We must be prepared and know how to deal with the inevitable. For this article, I am defining a relapse/lapse as any gluten exposure - be it blatant cheating or inadvertent/accidental. Over the years, I've crossed paths with far too many people with celiac disease and non-celiac gluten/wheat sensitivity who willingly and knowingly cheat. Of course, they have their "justifications," but in the long-run, they are cheating themselves, and their loved ones. If you're new to the gluten-free lifestyle, I'll be crystal clear - cheating is not an option for those with a gluten-related disorder. Accidental/incidental exposure is different from blatant cheating. Regardless of how or why we consume gluten - the damage is the same; the difference here is the intent. We must be mindful of these mishaps, so we do not continually repeat them. If we peel back the layers, there's probably a fine line between repeated accidental/incidental exposures and cheating. To be caught by surprise the first time is understandable, but if the same situation happens repeatedly - it shouldn’t be - we need to take a closer look at what’s going on.
GIG of ECW's "The Risks of Cheating" looks at the complications from repeated gluten exposures. bit.ly/GIGECW_Cheating
While we may not like visiting this stage, it can be beneficial to our overall success. It's important to view relapses/lapses not as failures, but rather another stage on our way to success. If we believe this set back is a failure, we're at risk of creating a self-fulfilling prophecy - undermining our efforts and making it easier to regress to our glutenous ways. Lapses reinforce our need to be completely gluten-free. Once we start feeling better, we might doubt gluten's role in our poor health. While having that piece of pizza when hanging out friends seemed like a good idea at the time, we are sorely and swiftly reminded why we began this transformation. We learn about resilience and persistence. When we are knocked down, we get back up and keep moving forward. Why? Because we deserve a better life and won't stop until we attain it. Because our friends and family deserve a better "us." Never give up.
"Courage does not always roar. Sometimes courage is the quiet voice at the end of the day saying, 'I will try again tomorrow." ― Mary Anne Radmacher
Ten Processes of Change The stages of change tell us what happens when we experience changes in thinking, emotion, and behavior, but the processes of change show us how the changes come to be. The implementation of these cognitive and behavioral activities are used to advance through the stages successfully. The processes are divided into two sections - Experiential and Behavioral. The experiential processes use increase over time and peaks in the contemplation or preparation stage and decrease in the action and maintenance stages. The behavioral processes are used most in the action and maintenance stages. This makes a lot of sense - first, we change our thinking, then we change our behavior.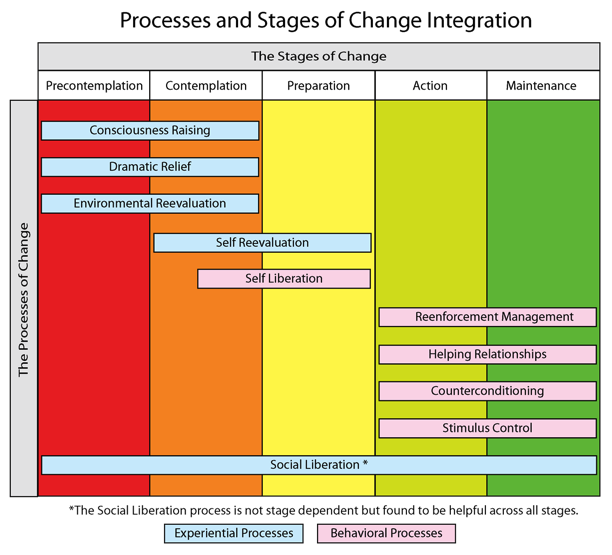
1. Consciousness Raising [Increasing awareness] - Experiential
Family members, medical professionals are telling us about our gluten intolerance and our need to be gluten-free. We start gathering information to get a better understanding of the new behavior required to remove gluten. "I recall information people have given me about gluten and gluten-related disorders."
2. Dramatic Relief [Emotional arousal] - ExperientialThe information we are receiving is concerning to us. We start to feel uncomfortable or possibly frightened. Maybe there's really something to this? "I react emotionally to warnings about gluten and gluten-related disorders. Grandma died from a stomach-related illness, no one really knew what it was. Could it have been celiac disease and she didn't know it? If I don't go gluten-free will the same thing happen to me?"
3. Environmental Reevaluation [Social reappraisal] - ExperientialWe're realizing our behavior is affecting those around us. The effect may be positive or negative depending on our choice. "I realize that if I continue to eat gluten and remain sick, I won't be able to care for my children. By being gluten-free, I am able to fully participate in life instead of watching it from the sidelines."
4. Self Reevaluation [Self-reappraisal] - ExperientialWe begin to look inward and assess how our gluten-free lifestyle is affecting us. We take note of how we are feeling physically and emotionally "I feel so much better when I'm gluten-free both physically and emotionally. I know I must remain so for life. When I cheat, I am disappointed in myself for putting my health and my family at risk."
5. Social Liberation [Environmental opportunities] - ExperientialAs we delve deeper into the gluten-free lifestyle, we find more people are aware of gluten-related disorders than we first expected. Grocery stores have dedicated aisles for gluten-free products. Select restaurants, bakeries, hotels, resorts, etc. have gluten-free offerings or specifically cater to the gluten-free community. [Note: Awareness of gluten and gluten-related disorders is growing. It's better than it used to be, but still has a long way to go.] "I find mainstream awareness is making it easier to be gluten-free. Family members who have been gluten-free for years tell me it's much easier to be gluten-free today than it was five or ten years ago."
6. Stimulus Control [Re-engineering] - BehavioralBy removing gluten from our homes [or at least moving and re-arranging it], we begin the mental re-wiring process. If gluten isn't there, we won't be tempted to eat it. Instead, we replace it with healthy, gluten-free alternatives "Whew! I feel more comfortable in my home now that gluten has been removed or sequestered. I'm also learning how to cope with gluten in situations where I don't have complete control [workplace, public venues, etc.]."
7. Helping Relationship [Supporting] - BehavioralHaving support is crucial to a successful transition. We need trusted individuals who are caring, compassionate, and willing to simply listen. "I have a spouse/friend/family member who is tremendously supportive. Always willing to listen and be my gluten-free champion." "My spouse/family members are horrible. They are unsupportive and at times overtly try to derail my efforts. Thank goodness for friends and my local support group members. They understand - they 'get it' - they keep me sane."
8. Counter Conditioning [Substituting] - BehavioralGrabbing a snack or something to eat can be one of those "autopilot" type actions. It's easy to snag a bag of chips, a cookie, or candy as we walk past it. Instead of stocking our kitchens with glutenous foods we supply it with healthy, gluten-free alternatives. We must be mindful, in today's gluten-free environment it's easy to swap out processed crappy glutenous foods with processed crappy gluten-free foods. Now is the time to make better choices - fresh fruits, veggies & gluten-free hummus, walnuts, almonds, cashews, hard-boiled eggs, high-quality gluten-free dark chocolate (Endangered Species Chocolate Bars). "I wasn't sure about it at first, but I find myself genuinely liking veggies and hummus as a snack."
9. Reinforcement Management [Rewarding] - BehavioralReinforcement Management renders consequences based on decisions and actions. While reinforcement can include the use of penalties, rewards tend to yield better results over punishments. A combination of cognitive and behavioral reinforcements, positive self-statements, and external recognition reinforce positive behavior and increase the likelihood of repeated positive behavior. While gluten-free treat food may seem like a reasonable reward option, it's not recommended to use any food as a reward (or punishment). Suggestions: Guilt-free "You Time," massage - mani/pedicure, a movie, museum trip, shopping trip, ballgame. "I really rocked it this week. My skills, knowledge, and confidence are growing. I found a gluten-free labeled food containing barley due to my label reading skills. I alerted the appropriate parties. My family and friends are noticing and praising me. I think I'll purchase that Wusthof Chef's knife, I've been eyeing up."
10. Self Liberation [Committing] - BehavioralWe believe change is needed and commit to making that change. "I can no longer ignore the facts. I have come to realize that I can and must be gluten-free. I know that it will not be easy, but I am ready to make the change for myself and loved ones."
James O. Prochaska, PHD
http://bit.ly/2BYGRuE
“James O. Prochaska is Director of Cancer Prevention Research Center and Professor of Clinical and Health Psychology at the University of Rhode Island. He is the author of over 400 publications, including three books, Changing for Good, Systems of Psychotherapy and The Transtheoretical Approach. He is internationally recognized for his work as a developer of the stage model of behavior change.”
Detailed Overview of the Transtheoretical Model
(Stages of Change)
http://bit.ly/2MCHnTR
ExperienceLife.com
“The Stages of Change”
By Jessie Sholl
http://bit.ly/2okF5dE
PsychCentral.com “Stages of Change”
By Mark S. Gold, MD
http://bit.ly/2LF8zwc
AConsciousRethink.com
“The 5 Stages Of Change Required To Make New Behaviors Stick For Good”
By Katie Uniacke
http://bit.ly/2NtydW8
Mood, Behavior, Mental Illness and Gluten

The intent here is not to bore you with medical mumbo jumbo [WARNING: medical mumbo jumbo lies ahead], but the takeaway here is simply this:
Gluten has been shown to affect mood, behavior, and cognitive function.
"The gut is not like Las Vegas. What happens in the gut, does not stay in the gut." ~ Dr. Alessio Fasano
Remember, gluten can affect any, and every organ in the human body – the brain and nervous system are not exempt – even without the presence of celiac disease. Science & medicine are discovering more connections as time goes on.
The statistics for mental illness in the United States are staggering.
- One in four [25%] adults experience mental illness in a given year.
- One in 17 [approx 6%] live with serious conditions like: schizophrenia, major depression, bipolar disorder.
- Approx. 1.1% of adults live with schizophrenia.
- Suicide is the tenth leading cause of death in the US (more common than homicide) and third leading cause for ages 15 to 24 year olds.
- More than 90% of those who die by suicide had one or more mental disorders
- In 2010, the Center for Disease Control reported 38,364 suicides per year – about 14% more than motor vehicle crashes.
- $193.2 billion – Lost earnings per year due to mental illness.
- Veterans account for 20% of suicides. 22 per day.
- Mood disorders (like depression) are the third most common cause of hospitalization for youth and adults 18 to 44.
After looking at those statistics, sadly, I suspect just about every family has had some experience with mental health issues in some form, be it directly or indirectly. I am no exception. My father was a diagnosed Paranoid Schizophrenic. Like many, he was not compliant with his medication regimen nor did he seek on-going professional help. The consequences of his choices are still rippling outward today, almost 50 years after his suicide. I will always wonder if removing gluten would've altered our family's history; without question it has altered my future.
Most mainstream medical professionals do not associate gluten with neurological/behavioral disorders. This is unfortunate because Dr. Marios Hadjivassiliou, Professor of Neurology at Sheffield, UK Teaching Hospitals, stated in 2002,“Gluten sensitivity can be primarily and at times exclusively a neurological disease.” http://bit.ly/1qXJdf3
Dr. Hadjivassiliou has done extensive work with a neurological condition called Gluten Ataxia. This condition is characterized by the loss of balance and coordination, visual disturbances, tremors, difficulty in walking. Living Without Feb/March 2011 has an excellent article on this topic - http://bit.ly/1u24c0q
Dr. Hadjivassiliou is not alone in his discoveries. Dr. Rodney Ford, a Pediatric Gastroenterologist/Allergist from Christchurch New Zealand, wrote this medical hypothesis paper in 2009 titled - “The Gluten Syndrome: A Neurological Disease” - http://bit.ly/1tkM58j
“Gluten can cause neurological harm through a combination of cross reacting antibodies, immune complex disease and direct toxicity. These nervous system affects include: dysregulation of the autonomic nervous system, cerebella ataxia, hypotonia, developmental delay, learning disorders, depression, migraine, and headache. If gluten is the putative harmful agent, then there is no requirement to invoke gut damage and nutritional deficiency to explain the myriad of the symptoms experienced by sufferers of celiac disease and gluten-sensitivity. This is called ‘‘The Gluten Syndrome” ~ Dr. Rodney Ford.
Dr. Ford has devoted an entire book on the subject of gluten's effect on our brains. I highly recommend “Gluten Brains” - http://bit.ly/GlutenBrains
“Neurologic and Psychiatric Manifestations of Celiac Disease and Gluten Sensitivity”was published in Psychiatric Quarterly in March 2012 and contains a great summary of a variety of gluten-related conditions. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3641836/
Neurologic Complications include:
- Gluten Ataxia
- Epilepsy and Seizure Disorders
- Peripheral Neuropathy
- Inflammatory Myopathies
- Myelopathies
- Headache
- Gluten Encephalopathy (Brain Damage)
- White matter abnormalities
Psychiatric Complications include:
- Anxiety Disorders
- Depression and Mood Disorders
- Attention Deficit-Hyperactivity Disorder (ADHD)
- Autism Spectrum Disorders
- Schizophrenia
The Celiac Disease Foundation created an excellent resource on celiac disease (and non-celiac wheat/gluten sensitivity) and mental health. It's meant to be shared with healthcare providers.
http://ow.ly/en1M30ghVy8
A wide range of psychological problems can arise for those with untreated celiac disease or non-celiac wheat sensitivity. Initially there may be a misdiagnosis of psychiatric illness due to some of the neurological and psychiatric symptoms that can be seen in untreated disease. Once diagnosed, there may be difficulty adjusting to a new diagnosis of chronic illness and adherence to a gluten-free diet."When a Mental Health Referral Is NeededA wide range of psychological problems can arise for patients with untreated celiac disease or non-celiac wheat sensitivity. These can include difficulties adjusting to a new diagnosis of chronic illness as well as dealing with adherence to a gluten-free diet and other aspects of disease management. Protracted duration of emotional or behavioral symptoms, greater severity of symptoms, and/or significant impairment in functioning are indicators of potential need for mental health treatment. These include:
• Finding little or no pleasure in life • Feeling worthless or extremely guilty • Crying a lot for no particular reason • Withdrawing from other people • Experiencing severe anxiety, panic or fear • Having big mood swings • Experiencing a change in eating or sleeping patterns • Having very low energy • Losing interest in hobbies or pleasurable activities • Having too much energy, having trouble concentrating or following through on plans • Feeling easily irritated or angry • Experiencing racing thoughts or agitation • Hearing voices or seeing images that other people do not experience • Believing that others are plotting against you • Wanting to harm yourself or someone elseWhen A Medical Evaluation Is NeededInitially those with celiac disease or non-celiac wheat sensitivity may be misdiagnosed with a psychiatric illness due to some of the neurological and psychiatric symptoms that can be seen in untreated disease including:• Mood changes • Anxiety • Fatigue • Difficulties with concentration and attention • Sleep difficulties • Decrease appetiteCeliac Disease and Gluten-Related Conditions Psychological Health Training ProgramThe Celiac Disease and Gluten-Related Conditions Psychological Health Training Program was created by the Children’s National Health System in partnership with Celiac Disease Foundation, and was made possible by a generous grant from the Resnick Family. This continuing education program provides a tool kit for medical and mental health practitioners to identify and treat patients living with celiac disease and other gluten-related conditions.Watch the Psychological Health Training Program Webinarhttp://bit.ly/2hI3QgTPsychological Health ManualAvailable both as an interactive manual and as a pdf document, the goal of this manual is to increase medical and mental health providers’ awareness of celiac disease and non-celiac wheat sensitivity in pediatric populations. However, it’s lessons apply to adult populations, and is a useful tool for patients and caregivers to better understand the disease.Read the Psychological Health Training Program Manualhttp://bit.ly/2iwf2wV
Depression
Depression is a medical condition that interferes with daily life; affecting thoughts, feelings, behavior, mood and physical health for extended periods of time. Some people may only have one episode of major depression in their lifetime, but often times it is a recurrent issue.
In celiac disease, nutritional deficiencies from intestinal damage may also contribute to depression. Lack of B-vitamins, specifically B-12 and folic acid have been linked.
Reports of depression in those with celiac disease began appearing in the 1980s. In 1982, a Swedish study reported “Our results suggest that depressive psychopathology is a feature of adult coeliac disease and may be a consequence of malabsorption” http://1.usa.gov/W3jKEB
A 1998 study shows about one third of diagnosed celiac patients also suffer from depression. Celiac adolescents have higher than normal rates of depression (31% vs 7% of adolescents without celiac). http://bit.ly/1qUGi2S
A large Swedish study published in 2007 compared almost 14,000 celiac patients against almost 67,000 healthy people. Researchers found that celiacs are 80% more likely to experience depression than the general population. They also looked at the celiac-depression relationship in reverse. They found those with depression had a 230% increased risk factor of having celiac disease. http://1.usa.gov/1pApGlN
Women with celiac disease have higher rates of depression than the general population. The risks were highest in those that were not compliant with the gluten-free diet. Even when compliant, women still had higher risks of depression over those without celiac. http://bit.ly/W3nKoE
According to Dr. Tom O'Bryan, children have a 40% increase risk of suicide. Those children with intestinal inflammation [no villi damage yet] have a 96% increased risk. http://bit.ly/1rJ7wjo
Adults diagnosed with celiac disease and/or intestinal inflammation have increased suicide risks as well. Another large study published in 2011 from Sweden shows those with with celiac disease [intestinal damage] had a 55% increased risk factor. Those with intestinal inflammation [no villi damage] had a 96% increased risk. http://1.usa.gov/Z4DFFk
More Gluten & Depression Studies
“A study has now demonstrated that gluten is independently associated with depression in patients with NCGS.” - http://1.usa.gov/1tZiAqc
“Exposure to gluten specifically induced current feelings of depression.” - http://1.usa.gov/1ucfDBZ
“Lifetime depressive symptoms may be present in one third of the CD patients who adhere to gluten-free diet. Long-term adherence to the gluten-free diet may reduce the risk of current depressive symptoms.” - http://1.usa.gov/1qqWZpe
Schizophrenia
Schizophrenia is a brain disorder that distorts thinking, behavior, emotions, the perception of reality. Delusions [believe people are try to control them or plotting against them] and hallucinations [hearing voices] are common symptoms.
There have been observations of Schizophrenia and gluten dating back to the 50's & 60's – also known then as “Bread Madness”.
In 1953 Dr Lauretta Bender started seeing increased incidences of celiac disease in those with childhood schizophrenia.
In 1961 Harold Graff, M.D. and Allen Handford M.D. published the case study, “Celiac Syndrome in the Case Histories of Five Schizophrenics”, about five patients with a history of schizophrenia and celiac disease who happened to be admitted to the same psychicatric hospital over the course of 365 days. A most curious observation in facility that had few admissions over the course of a typical year. http://bit.ly/1uFm56w
Dr. F. Curtis Dohan spent most of his career drawing connections between wheat and schizophrenia. He too noticed a number of patients with schizophrenia also had celiac disease – potentially 50 to 100 times the rate that would be expected by mere chance. Beyond these connections, he reported that a gluten-free diet improved some of the newly diagnosed schizophrenics, but not all. 2 out of 17 improved. http://bit.ly/1nhCHLw
In 1966 Dohan published “Wheat Consumption and Hospital Admissions for Schizophrenia During World War II”. He analyzed the the decreases in hospital admissions for schizophrenia during the wheat shortages in Finland, Norway, Sweden, Canada and the United States during World War II. http://bit.ly/1q0nRxU
Like many pioneers in their field, Dohan was often ridiculed and marginalized for his work [opioid research in mental illness], but he continued publishing his findings. Dohan also demonstrated that schizophrenia was almost non-existent in South Pacific cultures where little to no grains were consumed. When those cultures began to westernize their diet with the consumption of wheat, barley beer, and rice, the prevalence reached European levels. http://1.usa.gov/1wYpKja
Did Dohan find a “scientific smoking gun” linking gluten and schizophrenia – not exactly according to some experts, but his work is now proving to be quite interesting and now beginning to be validated.
It has only been over the last decade or so that experts have shown gluten's effects on the nervous system. Even to this day experts are still looking indisputable evidence connecting the two conditions.
In 2012, another study revealed that people with schizophrenia are much more likely than the general population to have an immune response to gluten. When those with schizophrenia and a documented immune response to gluten tried a gluten-free diet, they got better. These results are very promising for those suffering from a neuro-degenerative condition where little else works.
Not everyone with schizophrenia will see improvements on a gluten-free diet. New research is indicating about 20% may experience measurable improvements. Dr. Alessio Fasano's team have found that roughly 1 in 5 patients with schizophrenia have elevated levels of tTG6 (a new marker indicating gluten-sensitivity). Those patients put on a gluten-free diet were able to control their condition without medication. Promising results indeed!
More Gluten & Schizophrenia Studies
“Gluten Sensitivity and Schizophrenia” a PowerPoint presentation by Deanna Kelly, Pharm.D, BCPP Professor of Psychiatry at Univ. of Maryland School of Medicine.
http://bit.ly/2f4x8pv
“Emerging scientific literature contains several reports linking gluten sensitivity states with neuropsychiatric manifestations including autism, schizophrenia, and ataxia.” http://1.usa.gov/1tkxTvQ
“A drastic reduction, if not full remission, of schizophrenic symptoms after initiation of gluten withdrawal has been noted in a variety of studies. However, this occurs only in a subset of schizophrenic patients.” - http://bit.ly/2kIpUtQ
“Five biomarkers of gluten sensitivity were found to be significantly elevated in patients with non-affective psychoses (schizophrenia) compared to controls.” - http://1.usa.gov/1vXlWL1
Al Klapperich
Branch Manager
Gluten Intolerance Group of East Central WI
Updated: 11/05/17 - Add Celiac Disease Foundation information.
Updated: 02/12/17 - Fix broken schizophrenia study linkUpdated: 11/05/16 - Updated Deanna Kelly's presentation link.
Updated: 10/09/16 - Add Susan William's letter.